Division of BioTherapeutics
Formulation and Characterization of Vaccines
Vaccines are an extraordinary category of biopharmaceuticals. They are usually prophylactic and come in many types, from whole bacteria to peptides and nucleic acids. They are very cost effective and almost every human on the planet is vaccinated. The latter mandates that vaccines have to be extremely safe. Despite their success, vaccines are continuously subject to public debate. Vaccines tend to succumb to their success because they reduce disease whereas adverse effects, unavoidable to some extent, remain visible. Also, vaccines are not 100% effective. We try to unravel the mechanism of action of vaccines and to develop safe and effective administration and delivery concepts for vaccines.
Most vaccines are injected subcutaneously or intramuscularly. As vaccination programs expand slowly but continuously, the number of injections also increases. To avoid the disadvantages of injections with needles and syringes we develop alternatives. Acceptability of alternatives is often better, needle stick injuries are avoided as well as re-use of needles and syringes, which is still practiced in poorer parts of the world. Alternatives include dry matter high velocity projectiles, dermal as well as mucosal vaccination, e.g. via intranasal, sublingual en pulmonary routes.
Well defined, highly purified or synthetic antigens often lack the ability to activate the innate immune system. They need to be formulated in delivery systems in order to guide them to antigen presenting cells and lymphoid organs. In addition immune modulators are needed to activate antigen presenting cells via pattern recognition receptors. We develop these so called adjuvants and delivery systems for different immunization routes, e.g. mucosal and parenteral delivery. Examples of delivery systems are particles obtained from viruses (virus-like particles) or bacteria (outer membrane vesicles). Increasingly (semi-) synthetic approaches such as antigen-adjuvant conjugates are used in order to be able to understand the mode of action better and to steer the immune response in the direction needed.
In order to be able to modulate the immune response with the aid of delivery systems for antigens we need tools to analyse both the vaccine as well as the immune response in detail. To do this we develop and use physico-chemical and immunochemical techniques for antigen characterization. Complex vaccines like outer membrane vesicles, but also intermediates of vaccine production such as harvests from fermentors are being analysed by mass spectrometry based quantitative proteomics. An important rationale to develop robust procedures for vaccine characterization is the fact that current animal models to test vaccines often have limited value. They are expensive, often inaccurate, take a long time to perform and there are ethical dilemmas.
We try to improve our understanding of in vivo responses to pathogens and vaccines by introducing systems biology approaches. The combination of mass spectrometry based proteomics, transcriptome analysis and functional immunological assays like antibody measurements, cytokine multiplexing and FACS analysis gives unprecedented details about the response that vaccines induce (figure 1). More information from one experiment or one animal allows us to reduce the number of animals.
Even better than reduction and refinement is replacement of the use of animals in vaccine research. We are trying to achieve this, for example, by developing in vitro assays in which antigen degradation is mimicked as it occurs in antigen presenting cells. There are indications that the endosomal degradation pathway determines to some extent how immunogenic a protein antigen is. The aim is to develop easy to use (i.e. suitable for performance in routine QC labs) in vitro assays that can replace animal studies or at least can be used to demonstrate consistency between production batches.
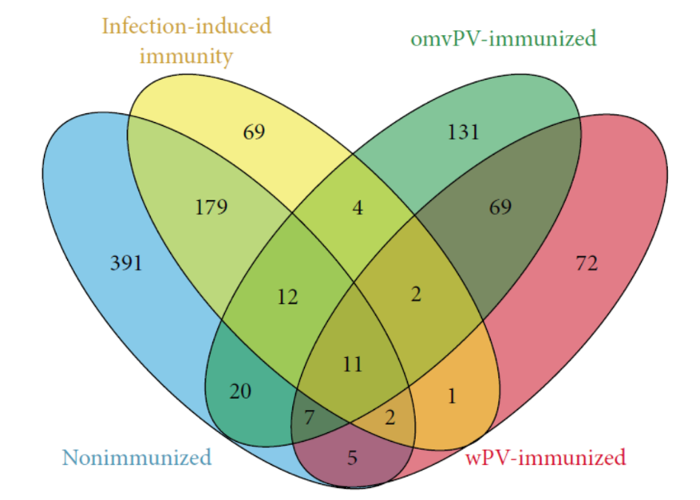
Figure 1. Differentially expressed genes in lungs of mice after a challenge with Bordetella pertussis bacteria. Mice were either naïve, previously infected or vaccinated with outer membrane vesicles or inactivated whole bacteria (Raeven et al., J Immunol Res 2017, doi.org/10.1155/2017/8512847).
Key publications
- Metz B., Michiels T., Uittenbogaard J., Danial M., Tilstra W., Meiring H.D., Hennink W.E., Crommelin D.J.A., Kersten G.F.A. & Jiskoot W. (2020), Identification of Formaldehyde-Induced Modifications in Diphtheria Toxin, Journal of Pharmaceutical Sciences 109(1): 543-557.
- Raeven R.H.M., Rockx-Brouwer D., Kanojia G., Maas L. van der , Bindels T.H.E., Have R. ten, Riet E. van, Metz B. & Kersten G.F.A. (2020), Intranasal immunization with outer membrane vesicle pertussis vaccine confers broad protection through mucosal IgA and Th17 responses, Scientific Reports 10(1): 7396.
- Michiels TJ.M., Tilstra W., Hamzink M.R.J., Ridder J.W. de, Danial M., Meiring H.D., Kersten G.F.A., Jiskoot W. & Metz B. (2020), Degradomics-based analysis of tetanus toxoids as a quality control assay, Vaccines 8(4): 712.
- Michiels T.J.M., Meiring H.D., Jiskoot W., Kersten G.F.A. & Metz B. (2020), Formaldehyde treatment of proteins enhances proteolytic degradation by the endo-lysosomal protease cathepsin S, Scientific Reports 10(1): 11535.

