
The QSPainRelief consortium will improve the treatment of chronic pain
The €6.24 million EU-funded research project QSPainRelief has kicked off. The project aims to help patients suffering from chronic pain with novel, personalised combinational treatments and is coordinated by Elizabeth de Lange from the Leiden Academic Center for Drug Research.
A major societal issue
Did you know that one out of five Europeans suffers from chronic pain? It can be both physically and emotionally debilitating and its socio-economic impact is huge: chronic pain patients are frequently absent from work or have to leave the workforce entirely due to their debilitating condition.
Therapy with a single medication is often ineffective and associated with substantial adverse effects. For example, opioids – a frequently used class of pain medications – are effective for some, but not all chronic pain patients. In addition, they may cause unwanted sedation, cognitive impairment, and liability of addiction and abuse. The project ‘Effective combinational treatment of chronic pain in individual patients, by an innovative quantitative systems pharmacology pain relief approach’, or QSPainRelief in short, aims to find a better treatment for chronic pain.

A new way
The consortium focuses on so-called combinational therapies of, for example, an opioid in combination with anti-anxiety or anti-depressant medications, or other existing medications that act beneficially on the central nervous system. These therapies may lead to an improved and healthier balance of therapeutic benefits versus adverse effects. ‘While already applied on a trial and error basis, the QSPainRelief consortium has a new approach to discover effective novel combination treatments of such existing drugs to improve pain relief in chronic pain patients. To that end we develop an in silico clinical trial approach that can systematically investigate all kinds of combinational therapies within a short time, as cannot be done clinical practice,’ project coordinator and Leiden professor Elizabeth de Lange says.
A personal approach
Novel technologies nowadays allow for much more personalised therapeutic approaches than in the past. One example is systems biology, which is based on a whole-body approach. Another field is pharmacogenetics, in which researchers study why and how people respond differently to certain medications based upon their individual genetic background. ‘And my own field aids to this as well,’ De Lange says. ‘In predictive pharmacology, we use computerised prediction and analysis of distribution and effects of medications in the body.’ Altogether, QSPainRelief merges these novel technologies to tailor treatments to the specific needs of individuals and stratified patients groups.
Consortium
The consortium is funded by the European Union’s Horizon 2020 programme. The ten institutions that collaborate in this multi-centre project are spread throughout Europe and include world-class experts on chronic pain, QSP computational pharmacological modelling, preclinical and clinical research, ethics, science communication, project management, and training of early-career scientists in academia, health care, and industry.
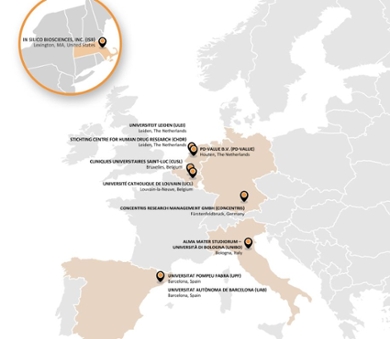
Partners
- Alma Mater Studiorum – Università di Bologna, Italy
- Cliniques universitaires Saint-Luc, Belgium
- concentris, Germany
- In Silico Biosciences, United States
- PD-value, The Netherlands
- Centre for Human Drug Research, The Netherlands
- Universitat Autònoma de Barcelona, Spain
- Universitat Pompeu Fabra, Spain
- Université catholique de Louvain, Belgium
- Leiden University, The Netherlands
For more information, see QSPainRelief's website
Header background image: ZEISS Microscopy
