
The Hague: working towards a healthier city
The disparities in terms of health and wellbeing in The Hague are considerable. A team headed by Jet Bussemaker, professor in the field of policy and society, wants to change that. The 'fences' in the healthcare system have to be got rid of. In particular the Laakkwartier and Moerwijs, two poorer areas of The Hague, should benefit from these changes.
This article was written before the outbreak of the corona crisis.

Lack of money, outdated houses, an unhealthy lifestyle and isolation. These are just some of the problems that are common in less prosperous neighbourhoods of The Hague, such as the Laakkwartier and Moerwijk, where a large proportion of the residents have a migrant background. The question is how we can improve people's health in these parts of the city. Professor Jet Bussemaker – Public Administration and LUMC/Medicine - and Annette de Boer, director of the Area Health Authority in The Hague (GGD), have launched the Healthy and Happy The Hague initiative (GGDH). Bussemaker's teaching remit is Science, Policy and Societal Impact, specifically in the healthcare sector.
Both Bussemaker and De Boer are keen to stress that GGDH is not simply a project. It is intended to be a long-term development, a movement that keeps on going. They describe the current image of healthcare and wellbeing in the city, populated by highly motivated professionals whose activities are strictly defined. The same applies for the flows of finance. The care sector is partly funded by the healthcare insurers, partly by the national government and partly by the municipalities, which are responsible for wellbeing in their local area. Nonetheless, it is important that healthcare and the social domain work in partnership, particularly given the close relationship between health and poverty. In parallel to these official bodies, there are also citizen initiatives in place, a number of which are very successful (see box).
Connecting people
Bussemaker's role is on the one hand to direct the process and on the other to carry out research during the process. 'The primary goal is to connect people,' Bussemaker explains. Actually removing the fences is something for the longer term, given that that calls for a complete change to the current system. ‘There's a lot to be gained in the meantime if the different parties actually know one another and can make referrals between them so that patients get the best possible help. This is what we're going to be working on first in Happy and Healthy The Hague.'

Focus
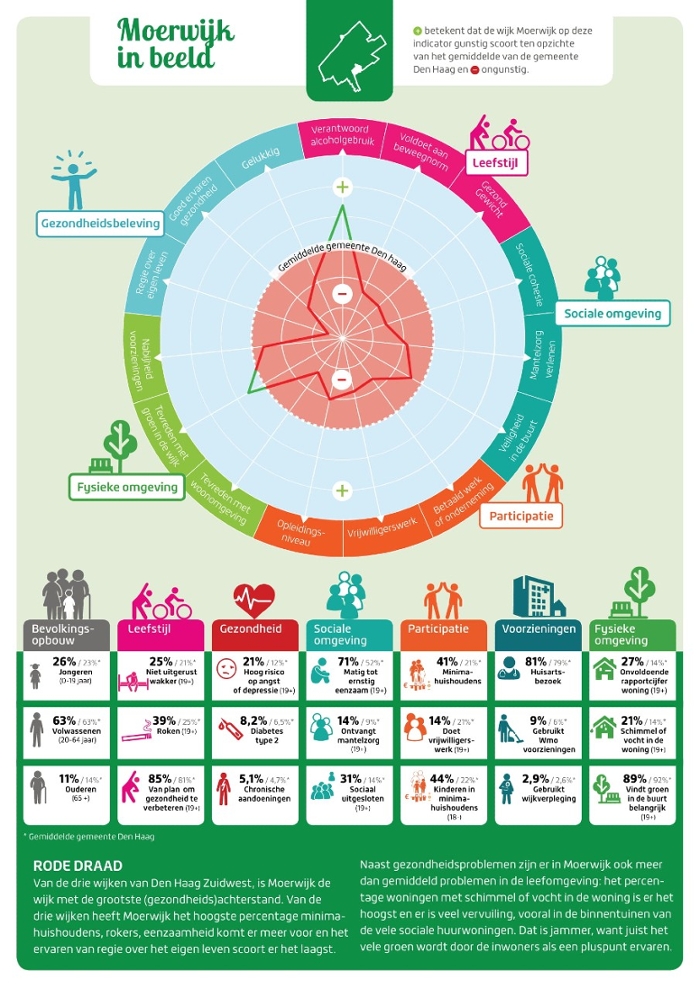
The focus of GGDH is currently on two neighbourhoods: Laakkwartier and Moerwijk. These are the areas of The Hague where health problems combined with social problems are the most serious. Within these neighbourhoods, the emphasis is on people with cardiovascular conditions, vulnerable elderly residents and susceptible people with multiple psychological conditions, who also have social and other problems.
Four theme groups have been set up to improve health and wellbeing, in which the people involved come together to discuss the issues; the parties include the municipal authorities in The Hague, the Foundation for Multi-agency Healthcare (a support organisation for healthcare providers in the Haaglanden region), citizen initiatives, healthcare insurers and knowledge institutions such as the University. The four themes are: Prevention, Redesigning Systems, E-health/ICT and Job Market and Education.
Change is essential
Annette de Boer is chair of the Prevention group. ' I am convinced that there are still a lot of benefits to be gained in these neighbourhoods in terms of health. We have to really listen to what motivates the healthcare professionals, what they believe is needed and what best suits the residents of The Hague. We need to take a broad approach that addresses problems like poverty and debt. And it's important that we guarantee the further development of the initiative so that we safeguard continuity.' Bussemaker: ‘If good healthcare is to remain achievable and affordable in the future, something fundamental has to change. Parties have to work together much more. Many care providers are already aware of that, and together with them we're creating a "community of the willing".’
Examples of private projects/citizen initiatives, including in The Hague
The National Diabetes Challenge, an initiative of former top volleyball player Bas van de Goor: to get people with diabetes moving more, they can sign up for a weekly walk, for twenty weeks. This initiative in The Hague is, unsurprisingly, The Hague Diabetes Challenge.
An initiative set up by general practitioners is Wellbeing on prescription. The key here is not to be too hasty in prescribing pills, but to take a broader approach. Could patients be suffering from problems of wellbeing that manifest themselves in physical complaints? In these cases, a better option would be to refer them to organisations that can help them with their problems. Whatever referrals are made, the GP continues to monitor the patient for several months.
Home-based elderly care aims to avoid elderly patients ending up unnecessarily in the emergency department or in hospital: district nurses offer vulnerable elderly patients more care and more complex treatments in their own homes. This will relieve the pressure on GPs and will avoid unnecessary visits to hospital by the elderly.
The Hague arteries: care providers, from specialists in hospital to GPs and district nurses, have made agreements about working together to treat patients with heart failure. Protocols have been drawn up detailing these agreements, stating clearly what each care provider has to do at what point in time in the process. This approach will be broadened in stages to include other cardiovascular conditions. The LUMC Campus The Hague is one of the partners in this initiative.
Complex operation
It won't necessarily be plain sailing. 'There are currently conflicting financial and administrative issues which make it into a kind of paradoxical Catch 22 situation,' Bussemaker explains. De Boer: ‘You need to get the professionals on board in changes that are good for the patient but where they themselves will also benefit. 'If fewer people end up in hospital as a result of Home-based elderly care (see box), that will have an effect on the earnings model of the specialists. Bussemaker: ‘I was talking recently with a director of a care home, who made the point that he, too, was an employer. We have to work together to come up with solutions.’ Bussemaker is happy with the current initiatives, such as those outlined here, that are not being imposed by the authorities, but that are being developed by enthusiastic citizens who are aware of the need for change. ‘It's important to bring people together,' says Bussemaker, 'and to involve them in these joint initiatives.'

Research
Bussemaker is closely involved in the research that aims to strengthen the GGDH. At this stage it is a matter of examining the figures. A lot of data is already available about the Laakkwartier and Moerwijk, including from research by the GGD and from practical experience with interventions. And we have already learned from the Hague Arteries project, for example, how many patients are expected to suffer from heart failure in the coming years. The effect of intensive collaboration on the numbers of patients and the costs has also been examined. Figures from the GGD on the health situation and wellbeing of the inhabitants of The Hague have formed the basis for the policies adopted by the municipality and the professionals working in the neighbourhoods. The municipality and other authorities are also keeping detailed records. The figures are being analysed by Bussemaker's colleague Jeroen Struijs from LUMC Campus The Hague. One of her PhD candidates is carrying out qualitative research: she is accompanying the professionals working in the neighbourhoods to study how they communicate with one another and with the local people. What do citizens consider good health?
Progress made
Bussemaker: ‘After a year, we now understand what are the biggest problems in Laakkwartier and Moerwijk, and we've made good progress.' But it doesn't end there. 'We're going to look at what makes projects successful, and why they work. GGDH is a continuous learning experience where we want to abandon the things that don't work and build further on positive experiences.'
See the complete factsheet for The Hague South-West
Text: Corine Hendriks
Mail the editors
